What is hepatitis? Types, symptoms, causes and treatment
> What is hepatitis?
The liver is a vital organ. It filters the blood, fights infections, and processes nutrients from the food we consume. Hepatitis is inflammation of the liver. It can be acute or chronic, with chronic hepatitis being much more common. Acute hepatitis is usually short-term and lasts for less than six months, while chronic hepatitis can last for years and involve complications such as cirrhosis and liver cancer.
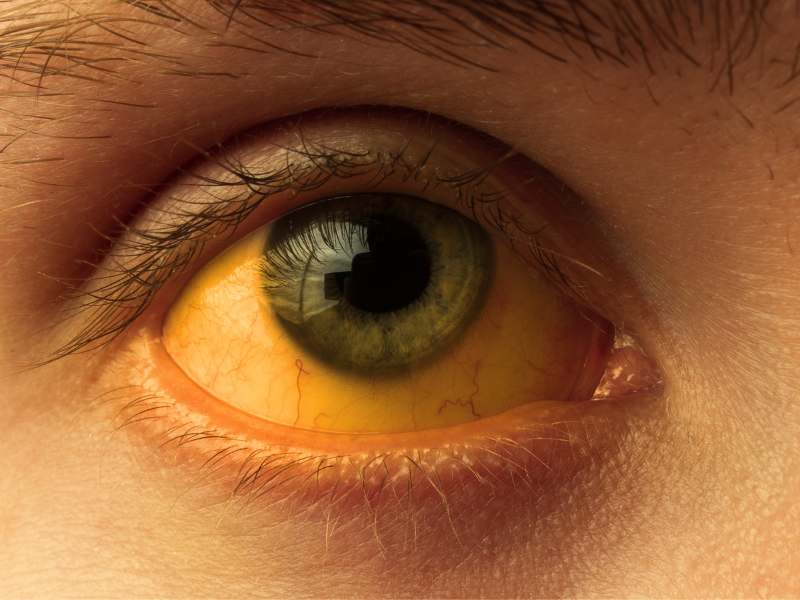
While hepatitis viruses are the most common cause of hepatitis in the world, heavy use of chemicals, drugs, and alcohol can also lead to hepatitis. An overactive Immune system or a genetic disorder can also be the cause of autoimmune hepatitis.
> Different types of hepatitis?
According to WHO, scientists have identified 5 main hepatitis viruses, referred to as types A, B, C, D, and E. These 5 types are of greatest concern because of their ability to cause chronic infections and liver cancer and possess the potential for outbreaks and epidemic spread. Type B and C in particular lead to chronic disease in millions as they spread due to transmission of body fluids or through contaminated food respectively. They are the most common cause of cancer and liver cirrhosis.
> Hepatitis A virus (HAV)
Type A is the most common type of hepatitis. It is caused due to consumption of food or drinks contaminated with the faeces of someone with the infection. This virus easily infects people in places with poor sanitation around the world. Nausea, dark urine, fatigue due to vomiting and fever, jaundice, and anorexia are some of the common symptoms of Hepatitis A. Most infections are mild in nature and effective vaccines are available to prevent HAV.
> Hepatitis B virus (HBV)
Type B hepatitis is usually spread through exposure to infective blood, semen, and other body fluids. It can also occur due to contaminated injections during medical procedures, and through injection drug use. Infants with HBV-infected mothers are at great risk of transmission at the time of birth. Healthcare workers who care for infected-HBV patients are also at risk due to accidental needle stick injuries. A mild illness, unease, and fatigue leading to anorexia are common symptoms of HBV.
Effective vaccines are available and are recommended to all infants, children or adolescents below the age of 19 for prevention.
> Hepatitis C virus (HCV)
HCV is the most common among IV drug users as it spreads through exposure to infective blood via contaminated needles or injections. Transmission can be parenteral, perinatal, and sexual as well. People who require frequent blood transfusions or organ transplants also fall under the high-risk category.
Most people show no symptoms of HCV infection but can experience abdominal pain, and bleeding/ bloating in the abdomen region. Nausea, loss of appetite and rapid weight loss are also observed in some cases. Unfortunately, there is no vaccine for HCV but can be treated with antiviral medication taken daily for two to six months.
> Hepatitis D virus (HDV)
HDV was discovered in 1977 and is structurally unrelated to the hepatitis A, B or C virus. HDV causes a unique infection that requires the assistance of viral particles from the hepatitis B virus (HBV). Simply put, infections occur only in those who are infected with HBV. The Hepatitis B vaccine does provide protection from HDV infection however, the dual infection can be very dangerous causing liver diseases and related complications. It is commonly observed among patients with a history of intravenous drug use.
> Hepatitis E virus (HEV)
HEV is also known as enteric (intestinal) hepatitis. It is very similar to hepatitis A and transmits through the consumption of contaminated water or food. It is generally not fatal, however, is a common cause of hepatitis outbreaks in developing nations across Africa and Asia.
Most patients develop HEV with no signs or symptoms. But, if you experience fatigue, myalgia (muscle pain), diarrhoea, nausea and/or vomiting, fever and cough or notice dark urine and light stool colour for more than two weeks, make sure you book an appointment with a gastroenterologist.
